The geek thinks: "Robot! Cool. What OS does it use? Is it on the network? Has anyone hacked this type of robot yet?"
I am that geek and I will get to those questions in a moment, but here's a question you need to be thinking about: Is it okay for a machine to slice into people and perform surgery, such as removing organs they no longer need? I'm thinking about this for several reasons, including my upcoming adrenalectomy and my job as a security researcher at ESET. But why do you need to think about this? Because robotic surgery is no longer science fiction: nearly half a million surgical procedures were performed robotically in North America in 2012.
So, there's a good chance that, if you need any one of a number of types of surgery in America today, your healthcare provider will want to use a robot. Are you okay with that? Clearly, most people will want to ask themselves: Does the surgeon's use of a robot increase or decrease the risks to me, the patient? In this post and others that I am planning to write, I hope to shed light on this question.
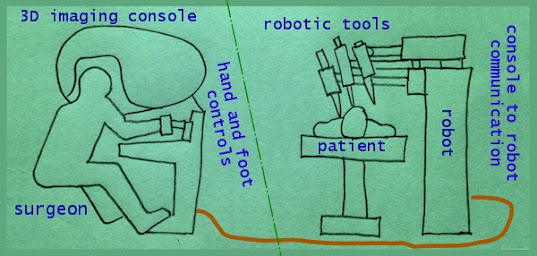
Note that I am not a doctor, nor am I a medical researcher, but I have some experience with risks related to digital technology. I work for a company that works to improve the safety of digital technology. A surgical robot is digital technology. Here's a simplified diagram of a robotic surgery setup:
The surgeon guides the robot tools from a 3D imaging console using hand and foot controls communicating over wires to the device. Note that the surgeon's console can be some distance from the patient (in telesurgery it could be miles away).
Slicing and dicing with da Vinci
If your healthcare provider does want to deploy a robot as part of your surgery there are a couple of data points we know already. First, the procedure is likely to take a bit longer. Second, the procedure will cost more. Third, the robot they will use is most likely to be the da Vinci Robotic Surgical System. The da Vinci is made by Intuitive Surgical, a company that went public 13 years ago at $9 a share [ISRG]. This was the same year the FDA approved the system for general laparoscopic surgery. Intuitive has since traded as high as $585.67, which might lead you to think that things are going well in robo-surgery land.Unfortunately, and I mean this sincerely as a fan of technology and a believer in the potential of robotics to improve our world, some things have not gone well. For example, according to one law firm:
there are now more than 4,500 complaints about the da Vinci surgical robot in the FDA’s MAUDE (“Manufacturer and User Facility Device Experience”) Database—50 or so of them involving the death of the patient—and 30 lawsuits against the manufacturer, Intuitive Surgical, Inc.You don't have to take a lawyer's word for this because MAUDE is on the Internet. and you can look up reports yourself (I count 500 reports involving Intuitive surgical so far this year). Bear in mind that reporting medical device problems to MAUDE is not mandatory, so there is no way to tell the actual number of problems with the da Vinci system.
Then came a bunch of studies examining the cost and efficacy of these million dollar marvels (yes, a da Vinci robot can cost over $1.5 million). Together with the lawsuits and media scrutiny, these have depressed share prices for ISRG, which is now trading around $430 with some analysts predicting values of $300 within the year.
Somewhat ironically, given my initial security geek reaction to the idea of a robot slicing into my flesh--fear of hacking--none of the problems with this particular technology cited so far have anything to do with malware, coding errors, comms failures, or hacking. The greatest risk factor right now, in my opinion? The impact of market forces on safety.
Sales pressure and medical devices
Intuitive is under tremendous pressure from shareholders to sell more robots and get more robotic surgeries performed. This leads to marketing tactics that oversell benefits and downplay risks. For example, Johns Hopkins research shows hospital websites making excessive use of industry-provided content to sell robotic surgery and overstate claims of robotic success. A CNBC investigation quoted Suraj Kalia, a Northland Capital analyst, in a recent report on the company:Our extensive field checks highlighted a story where aggressive marketing drives the message and true clinical utility seems secondary in nature.There is a lot of pressure on Intuitive to market the heck out of their product because a lot of doctors are now expressing doubts about the value of robotic surgery. Consider the blistering Statement on Robotic Surgery by James T. Breeden, MD, president of ACOG, the American College of Obstetricians and Gynecologists (with 56,000 members, ACOG is the nation’s leading group of physicians providing health care for women). Here's the short version: "there is no good data proving that robotic hysterectomy is even as good as—let alone better—than existing, and far less costly, minimally invasive alternatives."
Here are some of the figures that ACOG quotes:
At a price of more than $1.7 million per robot, $125,000 in annual maintenance costs, and up to $2,000 per surgery for the cost of single-use instruments, robotic surgery is the most expensive approach. A recent Journal of the American Medical Association study found that the percentage of hysterectomies performed robotically has jumped from less than 0.5% to nearly 10% over the past three years. A study of over 264,000 hysterectomy patients in 441 hospitals also found that robotics added an average of $2,000 per procedure without any demonstrable benefit...an estimated $960 million to $1.9 billion will be added to the health care system if robotic surgery is used for all hysterectomies each year.Between the medical questions and the growing number of lawsuits, Intuitive is under pressure, the kind of pressure that should, I believe, influence the way you interpret what people say about robotic surgery. Is the hospital pushing it on you? Is the hospital pushing it on the surgeon? Is the hospital skimping on robotic training, given the manufacturer's claim that surgeons are ready after two or three operations? Is the motive to achieve the best healthcare for you or is the motive a need to pay back the huge investment in hardware and supplies and maintenance contracts? Are doctors and hospital administrators being plied with luxury vacations and other perks to encourage them to use the robot more often in a wider range of procedures, including yours?
Those questions are currently more pressing than the need to analyze the da Vinci system's coding and connectivity. So far, I have found no indications that the system has been hacked and it does not appear to be connected to any networks. But that may change as the pressure to perform remote robotic surgery grows, powered by the perception that this can expand healthcare delivery at lower costs than training more surgeons. Already we see FDA approval for passive telemedicine robots. The term telesurgery has been coined and tests of procedures performed over the Internet are under way.
What's next for robotic risks?
In my next post I will break down the technical risk factors in more detail. These include analog issues, like build quality (here is a self-reported problem with da Vinci hardware that can cause burns), and also logical issues, like the security of device programming.I leave you now with a link to the AJOG report "The commercialization of robotic surgery: unsubstantiated marketing of gynecologic surgery by hospitals," and a link to a report that really rips into Intuitive. The author quotes a lot of sources that appear to check out. After reading it you are likely to question whether or not robotic surgery is right for you. As of now, I am going to ask my surgeon to take a more hands on approach.
[…] July 13, 2013: A geek worried about a robot? Robot or not? Robotic surgery and risk, part one […]
ReplyDelete